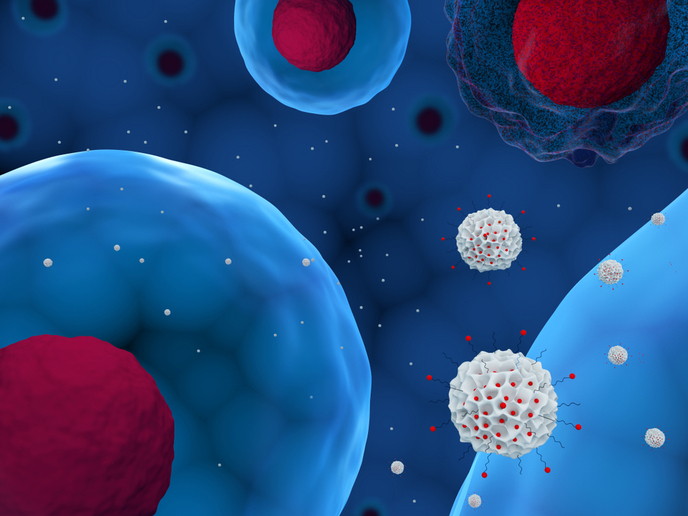
Nanovehicles transport drugs across biological barriers to the target site
Nanomedicine is a rapidly expanding field, offering the opportunity to significantly improve the efficiency of treatment and diagnosis of life-threatening diseases. Since many therapeutic targets are shielded behind biological barriers, reaching them with conventional drugs or diagnostic probes is often difficult. Training the next generation of researchers in nanomedicine To address the issue and facilitate the transport of drugs to specific organs or cells, the EU-funded NABBA(opens in new window) project proposed to develop nanoparticles. “Although nanocarriers is not a new concept, NABBA worked to improve the loading, selectivity and release of the drug to the target tissue,″ explains project coordinator Prof. Francesco Nicotra. The aim was to develop innovative nanoparticles capable of crossing various biological barriers including the blood brain barrier, and drive the drug to the pathological site. With the support of Marie Curie programme, NABBA established a network for training early-stage researchers (ESRs) in the multidisciplinary area of nanobiotechnology. Through a consortium of academic experts and industrial partners in the field, ΝΑΒΒΑ offered ESRs the opportunity to train in various technologies and industrial manufacturing platforms. Innovative nanoparticles for drug delivery NABBA ESRs employed various materials and approaches to chemically synthesise novel multifunctional nanoparticles. Advanced chemistry facilitated new synthetic strategies either for nanoparticle assembly or functionalisation. Functionalisation with specific biomolecules enables the nanoparticles to bind to specific sites and reach the microenvironment affected by different pathologies. Following extensive characterisation, scientists assessed the efficiency of loading, targeting and delivery of drugs or diagnostic probes as well as their pharmacokinetics in vivo. Particular emphasis was given to the molecular mechanisms governing biological barriers to find ways to overcome them for drug delivery. Covalent attachment of the drug to the polymeric component of the nanoparticle significantly increased drug loading efficiency and at the same time enabled the selective release of the drug at the pathological site. With respect to targeting cancer cells, one idea is to exploit the lower pH of tumours for drug release. An alternative approach uses irradiation with ultrasounds at the pathological site to break down the nanoparticles and release the drug. For crossing the inherently impermeable blood brain barrier, researchers have exploited the natural mechanism of transport using a specific membrane receptor. Conjugating a ligand of the LDL receptor at the surface of the nanoparticles led to significant increase of the transport of the drug into the brain. When used in an experimental model of Alzheimer’s disease, these nanoparticles reduced the amyloid plaques responsible for the condition and restored the memory in this mouse model. According to Prof. Nicotra, “this is one of the most significant achievements of the project, and the drug is currently being developed by our spinoff company.″ Overall, NABBA has successfully paved the way for new more effective therapeutics. Nanoparticle-based drugs will not only reach the target more efficiently but will require lower doses and thus cause fewer side effects. Given that biological pharmaceuticals, such as recombinant proteins, antibodies and gene therapy products face a bigger challenge crossing barriers, nanoparticles will continue to serve as delivery vehicles for these emerging medicines.