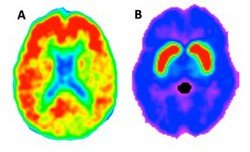
Imaging biomarkers for neurodegeneration
Recent research had revealed that the ageing brain undergoes prominent neurobiological changes such as white matter lesions, amyloid plaque build-up and decreased dopamine neurotransmitter function. Unfortunately, such changes are also seen in patients with neuropathologies such as dementia and Parkinson's, further complicating early diagnosis of disease. For instance, 20-50 % of clinically normal older people also have amyloid deposition in the brain, which is considered a hallmark pathology of Alzheimer’s disease. The EU-funded AMYDA (Disentangling the contributions of dopamine and amyloid burden to age-related changes in cognition and brain network connectivity in healthy older adults) project was initiated to find reliable imaging biomarkers of aging-related brain changes that can ultimately differentiate a “normal” brain from one that is in the preclinical stages of disease. AMYDA members assessed multiple imaging markers of the ageing brain using data form the Harvard Aging Brain study, collected at Harvard University and Massachusetts General Hospital. Surprisingly, results revealed that markers of white matter damage and markers of dopamine functions were not completely independent biomarkers of brain ageing. Mirroring the pattern for white matter damage, the dopamine system was found to be negatively impacted by high blood pressure. Also, studies confirmed that accumulation of cortical amyloid accelerates white matter damage, again suggesting that these markers are not separable and questioning the usefulness of studying these markers in isolation in the quest to diagnosing early Alzheimer's. Using techniques like functional magnetic resonance imaging (fMRI), researchers then explored the functional brain changes occurring in older individuals. The goal was to differentiate between healthy ageing and incipient neuropathology. Study outcomes revealed that biomarkers of fMRI functional connectivity were more sensitive and accurate than standard neuropsychological tests. In particular, fMRI of the midbrain–putamen functional connectivity in patients with Parkinson's disease revealed that this biomarker is proportional to the degree of neurodegeneration, providing hope that fMRI functional connectivity could be used as a biomarker of underlying neuropathology for early diagnosis. Results have already been published in over three journal articles. Given the steadily increasing elderly population, early detection and better treatment strategies are urgently needed as the socioeconomic burden of neurodegenerative disorders is extremely high. Further research exploiting human imaging to find neurodegenerative disease markers as well as therapeutic targets could help clinicians treat patients promptly and improve their quality of life.