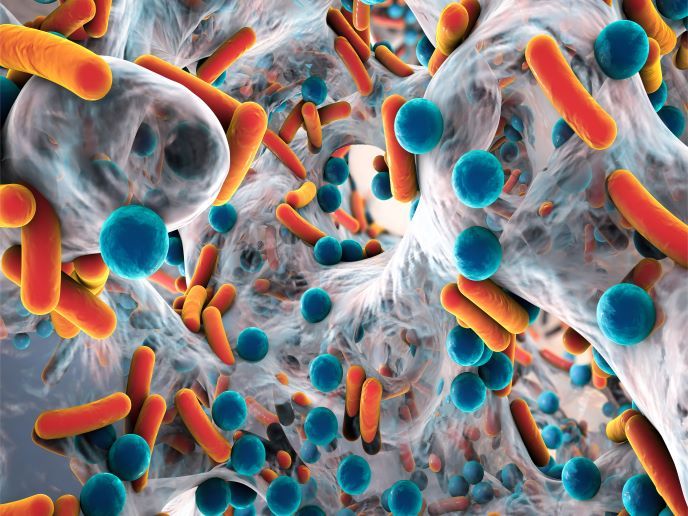
Love thy neighbour: how bacteria cooperate against an antibiotic threat
The European Commission has declared antibiotic resistance a major socio-economic challenge. Emerging evidence indicates that the environmental sector contributes to the spreading of antibiotic resistance, but the mechanisms remain poorly understood. Wastewater bacteria are well known to connect the human, animal and environmental sectors, so it is central to understand how antibiotic resistance spreads and circulates back to the human population.
Delineating bacterial interaction in biofilms
The scope of the SHARE_WW project was to study how bacteria growing together in specialised 3D communities known as biofilms(opens in new window) contribute to the transmission of resistance genes. The research was undertaken with the support of the Marie Skłodowska-Curie Actions (MSCA) programme and involved the co-culture of four different bacteria to generate multispecies biofilms. “In nature, bacteria do not live alone, as individual cells, but in microbial cities, as neighbours, interacting with each other in a friendly or competitive way,” explains the MSCA research fellow Ana Filipa Silva. The work focused on the resistance to beta-lactams(opens in new window), a widely used class of antibiotics, currently being exploited as the last resource in hospitals to treat multidrug-resistant infections. Bacteria detected in wastewater have been documented to degrade beta-lactams through the production of beta-lactamase enzymes which cleave the antibiotic chemical molecule, rendering it inefficient. To obtain a better understanding of the relationship between biofilm production and beta-lactam resistance, Silva investigated the impact of the antibiotic in bacterial organisation in the biofilm matrix. She discovered that bacteria that have preferred neighbours and biofilms are more stable when cooperation is established. In the presence of an antibiotic threat, biofilm matrix production increases to enclose sensitive bacteria and their neighbours in a dense and protective matrix. If antibiotic-resistant bacteria are present, then resistance genes are transferred to the sensitive species to protect them against the antibiotic. Moreover, resistant species seem to secrete to the surroundings the enzyme responsible for antibiotic degradation, thereby offering an additional layer of protection to their sensitive neighbours.
Targeting the neighbours: an alternative approach to tackling antibiotic resistance
Collectively, the work of the SHARE_WW project provided fundamental knowledge on biofilms resistant to beta-lactams in the environmental framework. “Importantly, our work unveiled the importance of all bacteria in biofilms – sensitive and resistant to antibiotics – in clinical diagnosis and treatment,” adds Silva. Bacteria in biofilms generate a cooperating community against the antibiotic threat, with resistant bacteria sharing resistance genes and enzymes while sensitive species build on a protective biofilm matrix. Understanding the conditions and the mechanisms underlying such events will fuel future research into strategies for eliminating antibiotic resistance from wastewater. Furthermore, this information has the potential to shift the focus of therapeutics from targeting only antibiotic-resistant bacteria to devising strategies against all species in a biofilm. Wastewater treatment plants have already shown interest in the SHARE_WW results and are working to incorporate the knowledge to develop tailored water treatments, especially when the treated effluent is recycled for anthropogenic activities.