Lab-grown immune cells forget lab culture shock
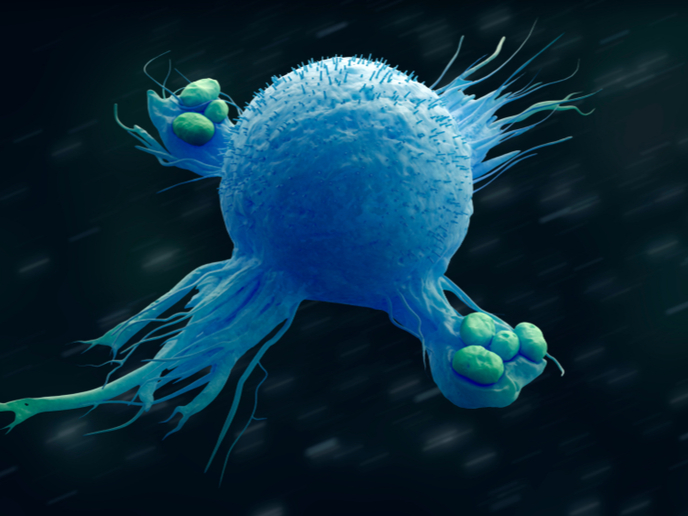
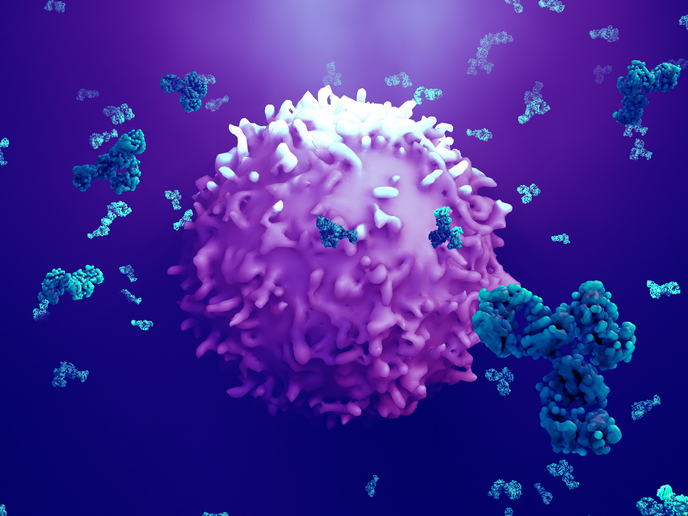
Macrophages are white blood cells that can be found in every body tissue. They are involved in a variety of immune functions: they surround and kill microorganisms, remove dead cells and stimulate the action of other immune cells. According to scientists, macrophages show promise as potential living drugs to fight infections, heal damaged organs and combat cancer. However, to be used for therapies, they need to be grown to big amounts in labs without losing their special functions. Is this even possible? Yes, according to researchers from Germany and France. Supported in part by the EU-funded MacAGE project, the research team has shown that macrophages grown in labs for long periods can function normally when transferred back into the body. Also, most importantly, they are no different than the cells that never left the lung tissue. The results show that cell therapies based on macrophages can, in fact, be developed in the future. The study(opens in new window) was published in the journal ‘Nature Immunology’. Cells grown in the lab are removed from their natural environment and the physical signals that seem essential to their function. They have to adapt to new conditions – plastic culture dishes and artificial nutrient solutions – which is “a real culture shock,” an article(opens in new window) posted on the website of MacAGE project host Technische Universität Dresden (TU Dresden), Germany, reports. “We wanted to know exactly how the cells change in prolonged cell culture and whether these changes are permanent or not,” states study senior author Prof. Michael Sieweke of TU Dresden in the news article.
Reversible changes
The team studied mouse macrophages that naturally live in the lung’s air sacs. They succeeded in growing these cells in the lab in volume over several months. The lab-grown macrophages did not look any different from their counterparts in the lung, but after examining them closely, the team noticed that the cells had actually undergone many changes to adapt to the new environment. “This was to be expected. Living on a plastic surface and having all the nutrients readily available is quite different from natural conditions. The cells had to get used to it and did so by changing the status of more than 3,000 genes. The question that truly interested us was whether these changes can be reversed,” explains Prof. Sieweke. To find the answer, the researchers transferred the lab-grown cells back into the mouse lungs. Detailed comparisons showed that the macrophages grown in laboratory conditions and those that never left the lung were now indistinguishable. “We were surprised to see that the substantial adaptations that the macrophages made to live in the laboratory have proven to be completely reversible,” remarks study co-lead author Clara Busch of TU Dresden. “The lab-cultured macrophages had forgotten about the time they spent in the lab and fully assumed their normal function and status in the lung, oblivious of their previous culture shock.” Although performed in mice, the research supported by MacAGE (Macrophage aging and rejuvenation) has very promising implications for human therapies, and it could be used to treat diseases such as cancer or infections similar to that caused by the SARS-CoV-2 virus. The project ends in December 2022. For more information, please see: MacAGE project(opens in new window)