New biosensors help control phenylketonuria disease
Phenylketonuria (PKU) is a rare birth defect that results in decreased metabolism of the amino acid phenylalanine. If left untreated, the disease can cause intellectual disabilities, seizures, mental disorders and behavioural problems. However, if detected early via new-born screening programmes, the disease can be managed via a strictly controlled diet. Unfortunately, due to a combination of the disease’s rarity, the complexity of testing, and the high costs of the required lab equipment, many hospitals in developing countries do not regularly screen for PKU. The issue is further complicated by the fact that home monitoring of blood phenylalanine levels is currently not feasible. The ERC-funded LABPATCH (Lab-in-a-patch for PKU self-assessment) project aims to change this by developing enzyme-based biosensors that can easily detect phenylalanine (L-Phe) levels – a leading indicator of PKU. “By lowering the cost of the materials used for the measurements, the LABPATCH biosensors will be accessible to hospitals and patients in developing countries,” says Paul Soto, a researcher with the project.
Two innovative biosensors
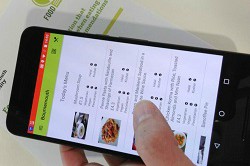
Building on the biosensor work done during a previous EU-funded project, LT-NRBS, LABPATCH researchers are now developing a spectrophotometric enzymatic biosensor and an electrochemical biosensor. Regarding the former, the enzymatic assays used to measure the concentration of L-Phe levels are performed in 96-well plates. This allows samples from multiple patients to be analysed simultaneously and using high-throughput, which in turn permits L-Phe levels to be monitored more frequently. “The biosensor demonstrates high sensitivity in the physiological range of L-Phe concentrations, meaning it can detect L-Phe levels associated with the onset of PKU,” explains project researcher, Morgane Valles. “The biosensor also makes use of immobilised enzymes, which increases its durability, ease-of-use and cost-efficiency.” As for the electrochemical biosensor, the patient wears this device at home as a patch. The patch contains electrodes modified with Phe-selective bioreceptors that automatically detect their sweat’s Phe levels in a non-invasive manner that does not require medical expertise or expensive facilities. The patch is connected to a miniaturised control unit for electrode operation and wireless data transmission to an external device (i.e. smartphone or tablet). Validated on anonymised human blood samples spiked with different phenylalanine concentrations, the LABPATCH biosensors were found to be reproducible between sample batches.
Making early detection more accessible
By developing low-cost, easy-to-use biosensors, the LABPATCH project is well-positioned to have a big impact on PKU detection in developing countries. “Typically, blood Phe concentrations are only analysed in specialised laboratories and at a frequency of just once or twice a month,” says project researcher Rafael Artuch. “But with LABPATCH, patients can control Phe levels at home, giving doctors the data they need to better control the disease.” Despite these successes, project researchers note that there is room for improvement, particularly as to the reproducibility and chemical and thermal instability of the biosensors. “These inherent technological drawbacks of enzyme-based sensors can be mitigated through adequate biosensor characterisation and through protein engineering,” adds Soto. “These improvements will be the focus of the next phase of the project.”