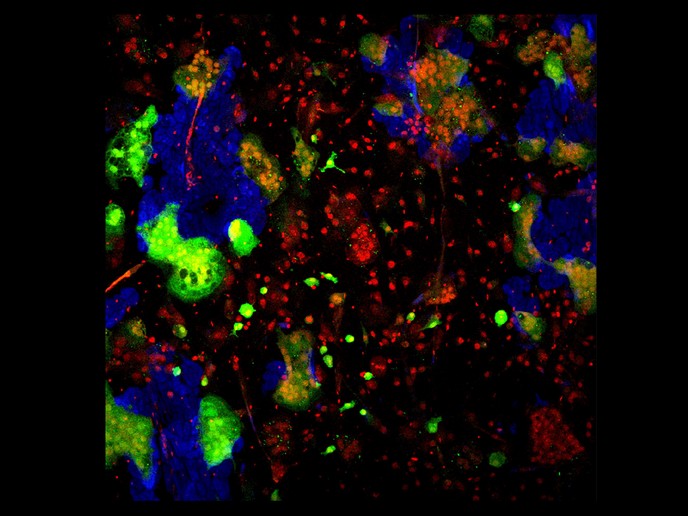
Bone-eating giant cell provides clues to brittle bones and other disorders
Bone-related diseases are the most common cause of severe long-term pain and reduced quality of life for millions of people. They include osteoporosis, periodontitis and rheumatoid arthritis – the number of people suffering from these conditions is set to increase substantially as Europe’s population ages. The EU-funded EUROCLAST(opens in new window) (Exploring Functional and Developmental Osteoclast Heterogeneity in Health and Disease) project brought together over 30 specialists, including around a dozen PhD students from 7 institutions and 2 companies, to examine cells known as osteoclasts. These cells are responsible for bone degradation which is important for skeletal renewal and repair. Most cells in the body have just one nucleus, but certain mononuclear cells fuse to form the super-large osteoclast cells which attach themselves to mineralised tissues such as bone and digest them. “All mineralised tissues can be digested by this cell,” explains project coordinator Vincent Everts, a recently retired professor at the Vrije Universiteit Amsterdam in the Netherlands. Investigating the precursor cells known as monocytes which fuse to form osteoclasts, “we found that osteoclasts differ according to the bone they digest or degrade. For instance, there is an osteoclast associated with the skull bone and a functionally different one associated with the long bones in the arm or leg,” Professor Everts says. This is important in order to understand osteoclast effects in different disease states, occurring at different skeletal sites in the body. Osteoclast activity Osteoclasts lower the external pH (acidity) when attached to bone tissue which results in the mineral (calcium phosphate) being dissolved. This process is followed by the secretion of a number of enzymes that digest proteins in the bone. Too much osteoclast activity can result in lower bone density and brittleness as, for example, in osteoporosis patients. By contrast, decreased osteoclast activity results in high bone density, as seen in the disease osteopetrosis where the bone becomes denser and hardens. “While this disease is rare, many key regulators of osteoclast activity have been identified by studying this terrible condition,” says Professor Everts. Researchers were able to visualise this cell type using new types of electron microscopes used in other fields, which, in effect, slice the cell into a large number of sections producing a series of micrographs. “Previously we were never able to visualise the inside of the cell in such detail but now we see what’s happening at different locations within it,” he says. A metabolic-labelling system was developed by the researchers to track how molecules and intracellular structures move and function within the giant cell, providing information on how bone degradation occurs, and which parts of the cell are actively involved in this digestion. Assays and cell discovery Special assays were developed to analyse osteoclast activity in human serum – blood taken from patients – and investigate the enzymes expressed solely by these osteoclasts. This specific enzyme analysis technique is now being commercialised for diagnostic use. The group’s research also contributed to the discovery of cells that resemble osteoclasts. “The osteoclast is very difficult to culture and cannot be kept alive for very long,” Professor Everts explains, “but if you have a cell that resembles the osteoclast, you can investigate osteoclast-like activity and the effect of inhibitors on these cells, or, alternatively, the effect of stimulating compounds, thus providing tools to investigate in detail how these cells function under normal and pathological conditions.” Such insights could pave the way for new diagnostic tools and therapies.