Functional neuroimaging reveals preclinical alterations in brain function
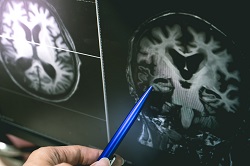
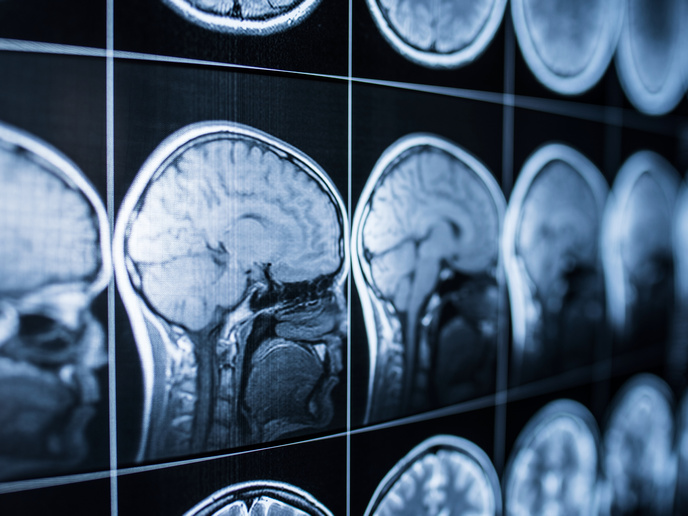
AD poses one of the biggest health challenges of our time. More than 10 million people are currently affected by dementia in Europe and by 2030 the number of new cases will exceed 13 million. Due to patients’ need for continuous support over several years, the sustainability of the global healthcare infrastructure is at stake. Once symptoms such as memory impairment and brain atrophy become apparent, the disease is already too advanced. The majority of future cases are already affected by the silent stage of AD that can last up to 20 years. Current methods for detecting the disease, such as positron emission tomography, are invasive and therefore unsuitable for screening the aging population at large. As a result, NPAD has developed neurofeedback technology for the prevention of AD. The project established a non-invasive paradigm for learning to self-regulate brain activity. The researchers used functional magnetic resonance imaging (fMRI) and developed real-time processing and virtual reality (VR) software, to quantify neurofeedback performance in a standardised manner. The goal was to derive a neurofeedback performance endophenotype (NPEP). Measuring brain function in AD The NPEP was derived from 63 subjects at risk for AD, through medical profiling via multi-modal neuroimaging, cognitive, genetic and biomarker data. These were assessed diagnostically via the application of advanced graph theory and statistical modelling methods. “We utilised a 30-minute real-time fMRI session, during which subjects received continuous neurofeedback within a VR environment. The aim was to reduce activity in the hippocampus, a crucial brain region,” says Dr Stavros Skouras, the principal investigator of NPAD, a Marie Skłodowska-Curie fellow. “We had to develop in-house software due to the lack of readily available solutions, compatible with the latest MRI technology, to obtain the brain data in real-time and perform the project,” highlights Dr Skouras. The designed paradigm allowed the extraction of subtle metrics associated with genetic predisposition to AD, neurodevelopmental processes and disease symptoms; such as apolipoprotein e4 genotype, hippocampal structural connectivity and memory impairment, respectively. An economic, non-invasive, pre-screening method for AD NPAD results suggest specific patterns of alterations in brain function, for the detection of the preclinical stage and for monitoring clinical progression and therapeutic efficacy in AD. “These metrics can be used as novel indicators of memory function and are unbiased with regards to self-reporting limitations of psychometric questionnaires. They can further help differentiate, in terms of the alterations in brain function, between Alzheimer’s disease and healthy aging,” states Dr Skouras. The developed methods hold potential for scalable prognostic screening and translational applications. For instance, clinical trials can use the developed procedure to pre-screen participants, leading to significant cost reductions. The procedure also offers a standardised method for quantifying and monitoring the therapeutic efficacy of clinical interventions. The NPAD project has opened new avenues for personalised medicine applications. These will eventually enable commercial applications for self-training and strengthening neural reserve and resilience to AD. “An important merit of our approach is that it aims to transform a medical examination into a non-invasive, entertaining video-game controlled with the mind. In this sense, we are aiming to create future clinical applications that are not only safe but also enjoyable for the patient. However, before any such service becomes a reality, further R&D is necessary,” concludes Dr Skouras.