Cerebral organoid models of viral infections offer insights into human brain development
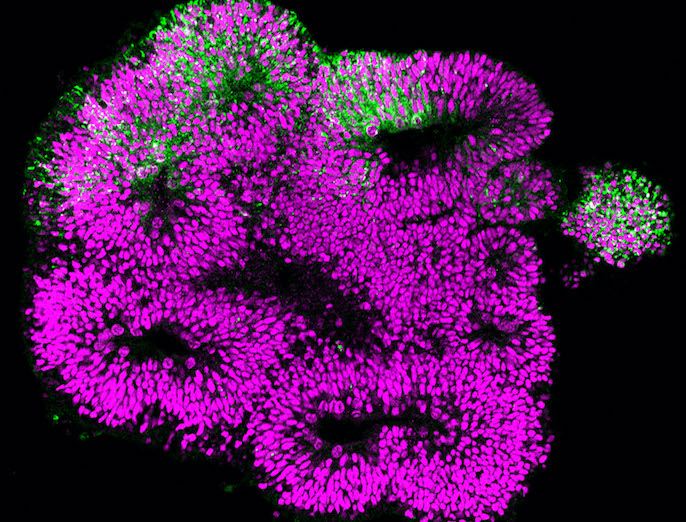
While studying model organisms, such as mice, has provided researchers with valuable insights into the underlying principles of human brain development, some mechanisms appear to be unique to our species. The EU-supported Spindle Brain Organoid project used cerebral organoids(opens in new window) (three dimensional organic structures comprising human neural stem cells and neurons) to investigate brain development. The project used organoid models to study viral infections in the brain, investigating how viruses can target human neural stem cells and so compromise their ability to generate neurons. The findings help explain how viral infections can damage the foetal brain and why these infections are particularly dangerous during pregnancy. Through these infection models, it is now possible to better understand how viruses spread within the brain and to develop strategies to limit the infections, and to help design selective antiviral therapies. This research was undertaken with the support of the Marie Skłodowska-Curie programme.
Neurogenesis in a dish
The 3D cerebral organoid in vitro modelling technique, developed in the Knoblich laboratory(opens in new window) which hosted the project, can replicate some of the mechanisms of human neurogenesis. This includes the differentiation pathways by which pluripotent stem cells start to specialise. Neural stem cells are present early on in development and remain through several rounds of cell division, giving rise to all the neurons of the brain. Crucially, cerebral organoids are not only an important source of human neural stem cells and neurons, but also reproduce the spatial organisation of cells that is seen in the developing brain. This provides a powerful model of the human brain. “The technique is also amenable to experimental manipulation and human gene editing, so can be used to functionally test the roles of human genes and human genetic defects in the process of neurogenesis,” adds Veronica Krenn, research fellow.
Introducing the viral loads
Guided by the discovery that the Zika virus(opens in new window) could target human neural stem cells and alter their behaviour during neurogenesis, causing microcephaly (small head) in newborns, the researchers introduced viral infections to cerebral organoid models to trace their impact. Immunohistochemical analysis on control and infected organoids was used to identify where the stem cells were, also which cells were infected and what impact the infection had on them, for example whether they were killed during the infection. The team tested the ability of viruses, including Zika, to infect organoids and target neural stem cells, as well as the effect of such infections on neural stem cell survival and behaviour, and organoid growth. They also investigated the antiviral mechanisms that neural stem cells adopt to fight infection. “These models can be used to study various infections and identify strategies to limit viral spreading to reduce the neurological damage caused by these infections,” says Krenn. “Further testing using our in vitro models could help uncover new antiviral drug therapies to prevent neurological complications associated with these infections.” The next step will be to use these different infection platforms to develop virus-specific therapies to combat infections and to limit brain damage.