Studying antibiotic resistance
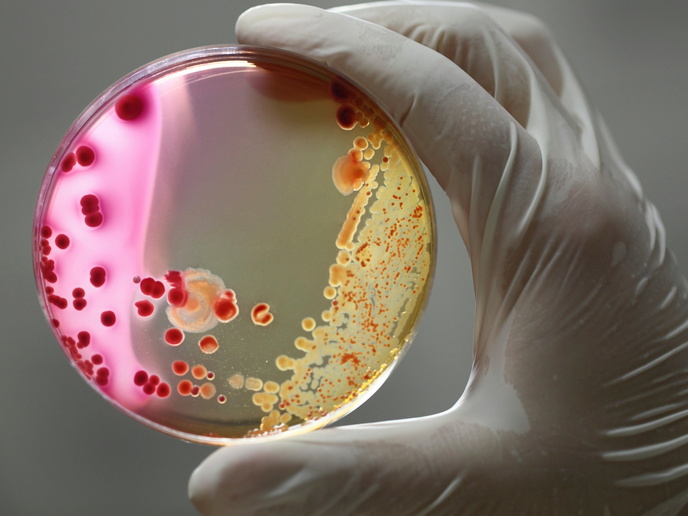
Antimicrobial resistance is rapidly becoming a major health issue, especially regarding bacteria that cause health care- and community-acquired infections. Apart from a significant health care burden, antimicrobial resistance hampers therapy and necessitates the development of novel treatments. As a result, we need to understand how judicious antibiotic use and selection pressure impact the emergence of resistant bacteria. Seeking to address this, the EU-funded 'Impact of specific antibiotic therapies on the prevalence of human host resistant bacteria' (SATURN)(opens in new window) project performed molecular and patient-level investigations. The generated information should help clinicians make evidence-based decisions on therapeutic management and antibiotics prescriptions. The consortium performed intervention and observational clinical studies to generate evidence on how antibiotic exposure affects the acquisition, selection and transmission of antibiotic-resistant bacterial species within hospitals. The studies investigated the impact of the duration and dosage of treatment of various antibiotics on resistance, in the community, general hospital wards and intensive care units. Over 5 300 patients were enrolled in these studies. Ongoing analysis of the results should reveal critical molecular and pharmacologic parameters of the virulence and fitness of resistant strains. Furthermore, the SATURN project made significant methodological advances towards the reliable detection of resistant bacteria. Taken together, SATURN's tools and observations should form the basis for better antibiotic-prescribing practices and help propose courses of action to prevent spreading of resistant strains.