New verification system delivers radiotherapy treatment safely to cancer patients
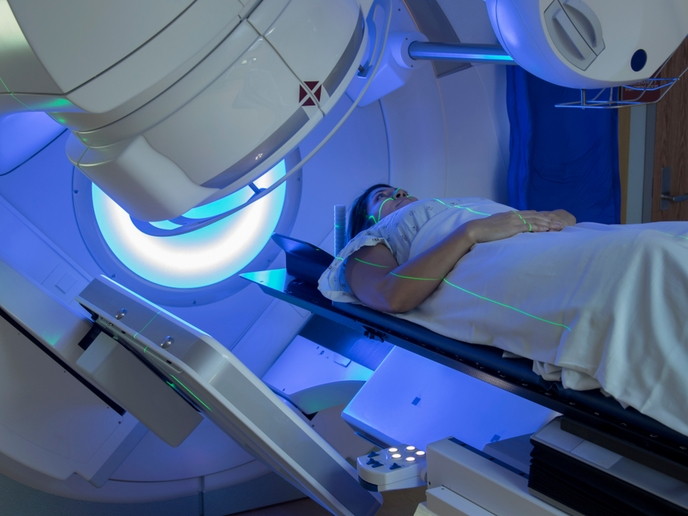
Radiation therapy is a localised treatment that uses beams of ionising radiation such as X rays delivered by a linear accelerator to kill cancer cells and shrink tumours. However, the immediate proximity of tumours to healthy tissues requires precise execution to avoid damaging normal tissue as well. A new solution to personalise every radiotherapy treatment The EU-funded KERMA project provides a new service to improve quality assurance and reduce collateral effects in radiotherapy. The service is based on a disruptive technology and offers personalised radiotherapy treatment, optimising the dose and the delivered location. Moreover, the technology provides three-dimensional dose maps, thereby reducing errors in patient’s treatments. “The overarching aim was to help decision-making by physicians and thus, apply radiation treatment more safely and quickly,″ explains project coordinator Dr Mari Carmen Ovejero Mayoral. CT scans provide the position and extent of gross tumour, also known as gross target volume (GTV). The margin around the tumour is considered for sub-clinical disease spread and cannot be fully imaged but must be treated to achieve cure. This is known as the clinical target volume (CTV) and varies from patient to patient. Radiotherapy planning must allow for uncertainties of delivering the right dose to the CTV, a geometric concept known as planning target volume (PTV). Radiotherapists have to evaluate the risks and ensure that the nearby tissue or organ doesn’t receive a dose that isn’t safe. In addition, tumour staging is often necessary to decide on whether to include localised lymph nodes in the treatment strategy. Treatment plans calculate the route of each beam and how the therapy system will deliver radiation. They compute the expected dose distribution in the patient’s tissue taking into account the type of tissue to be penetrated while at the same time avoiding critical structures. The future of radiotherapy planning Although the concepts of GTV, CTV and PTV have been enormously helpful for the development of treatment protocols, they rely on high quality imaging of the tumour and the surrounding anatomy. KERMA has been designed to assist in the calculation and verification of the radiotherapy treatment before it is delivered to the patient. The design of novel software not only allows data acquisition but also automates the entire process. KERMA provides a novel service based on a platform which integrates and automates all the radiotherapy treatment workflow. This includes dose verification, error reduction and performance improvement. Preclinical testing of the prototype has produced encouraging results, fuelling the validation of KERMA in a clinical setting. Imaging techniques have advanced over the years providing more precise gross tumour estimates and CTV margins. Technological developments and molecular imaging techniques are expected to enhance radiotherapy planning and precision in the future, further supporting its usefulness in cancer therapy. Given that radiotherapy is applied to more than 50 % of cancer patients, there is no room for errors in treatment execution. Dr Ovejero is confident that “KERMA will contribute to more accurate radiotherapy planning and safer treatment delivery to cancer patients.″