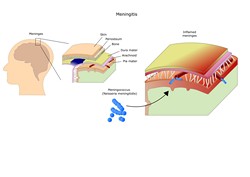
Molecular insight into meningitis
Neisseria meningitidis constitutes the major cause of bacterial meningitis and septicaemia worldwide. The animal models utilised so far to study N. meningitidis infection have not accurately reproduced the key features of meningococcal disease such as skin lesions and purpura. To address this, scientists on the EU-funded HUVASC-SEQ (Functional Genomics Analysis of Neisseria meningitidis interactions with human dermal blood vessels in vivo) project developed a humanised mouse model for meningococcal infection, which reproduced the skin and purpuric lesions associated with meningococcal septic shock. This model entailed the transplantation of human skin onto immunodeficient mice followed by inoculation of N. meningitidis into the blood circulation. The pathogen migrated specifically to the human endothelium present in the skin graft, establishing micro-colonies and colonising the vascular endothelium. Ultimately, this process led to an inflammatory response, tissue damage and formation of purpuric lesions like those seen in humans with acute meningococcaemia. During HUVASC-SEQ, researchers performed genome-wide analysis and used functional assays to gain a better understanding of the mechanisms of vascular colonisation and meningococcal disease in vivo. They successfully identified new gene candidates important for virulence during the process of vascular colonisation. Overall, the study findings provided fundamental new insight into the pathogenesis of N. meningitidis. Future research using the N. meningitidis humanised mouse model should help scientists better understand vascular leakage and how N. meningitidis crosses the blood brain barrier to cause meningitis. Collectively, these efforts will lead to the development of novel therapeutics.