‘Nose to knee’ – a novel way to repair knee joints
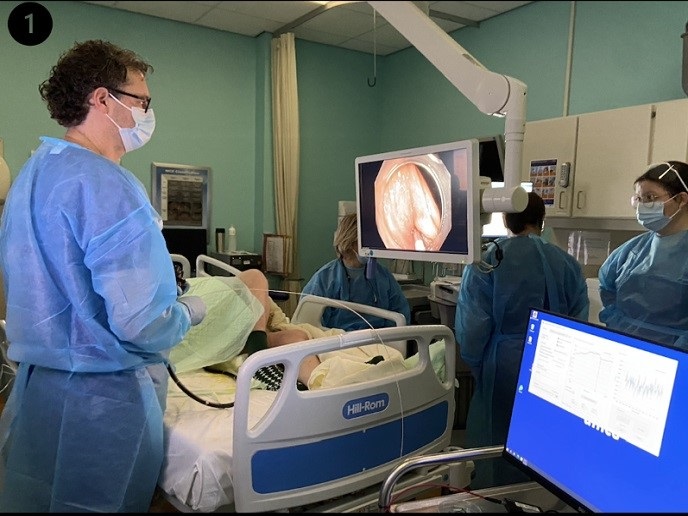
Damage to the cartilage of the knees can be painful and debilitating. Scientists from the BIO-CHIP(opens in new window) project have developed a new ‘nose to knee’ technique which uses cartilage taken from between the nostrils to repair knee joint lesions. “We take a small biopsy from the nasal septum under local anaesthetic,” explains project coordinator Anke Wixmerten, whose project was supported by the EU. “From that biopsy we isolate the cells and grow them in the lab. Once we have enough cells, we generate a large cartilage graft that can be implanted in the knee.” Wixmerten, responsible for quality assurance and regulatory affairs at the Department of Biomedicine, University of Basel(opens in new window), Switzerland, adds: “Different cell-based treatments are currently available for cartilage repair, but they are not tissue like the nasal cartilage.”
Microfracture repair
The approach has another advantage. “Nasal cartilage cells have been shown in the lab to be more efficient in proliferating than the cells from the joint, and produce cartilage of good quality,” says Wixmerten. “Their properties are more reproducible, and therefore the quality of the cartilage is less variable.” The process can create tissue of up to 12 square centimetres and treat a defect of up to 8 square centimetres. Such large areas of damage cannot be treated successfully with the common procedure known as ‘microfracture’, in which small holes are made in the joint bone surface to attract bone marrow stem cells, which repair the cartilage. Microfracture works well in the short term, but the repair cartilage is of poor quality and the pain often comes back over time. “You need to look at the longer-term results – up to 5 years and more – to see if there is actual benefit from the tissue,” Wixmerten notes. She adds: “Microfracture works best for young patients and for small defects – up to around 2-4 square centimetres. But larger defects, and revision surgeries for patients whose previous surgical treatment failed, are still a challenge.” The Phase II clinical trial at the University Hospital Basel(opens in new window) and four other clinical centres enrolled over 100 patients. Of these, 98 received the ‘nose to knee’ treatment. Patients are being assessed 1 and 2 years after the treatment.
Volleyball videos
“What we have seen so far is that the procedure is safe, and most patients benefit considerably from the treatment,” Wixmerten says. Patients’ self-assessed clinical scores of post-operation mobility significantly increased and they could return to their favourite sports activities. “Patients have been sending us videos and pictures where they went snowshoeing or skiing, playing volleyball or jogging only a year after surgery,” she adds. For regulatory reasons, only younger patients up to age 65 were included in the clinical trial. “We hope that with the repair of cartilage lesions, the risk of developing osteoarthritis can be decreased or postponed,” Wixmerten explains. The team now has temporary authorisation in Switzerland to include patients with patellofemoral osteoarthritis, in which cartilage behind the kneecap is worn away, and for use of the procedure in other joints such as the ankle or shoulder. Osteoarthritis is a challenging condition, since it is often accompanied by inflammation. “We know that tissue engineered in the lab from nasal cartilage can withstand inflammation better than tissue-engineered cartilage from the joints, at least in experimental settings. So we think it could work for osteoarthritis,” Wixmerten says.