Online tool targets cost-effective childhood screening
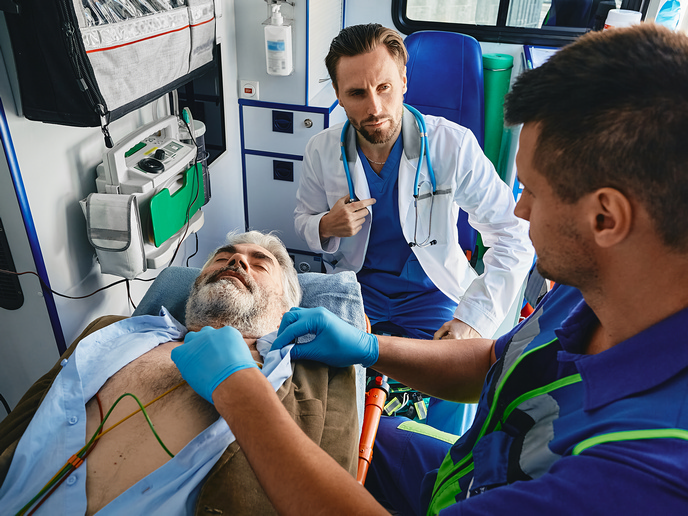
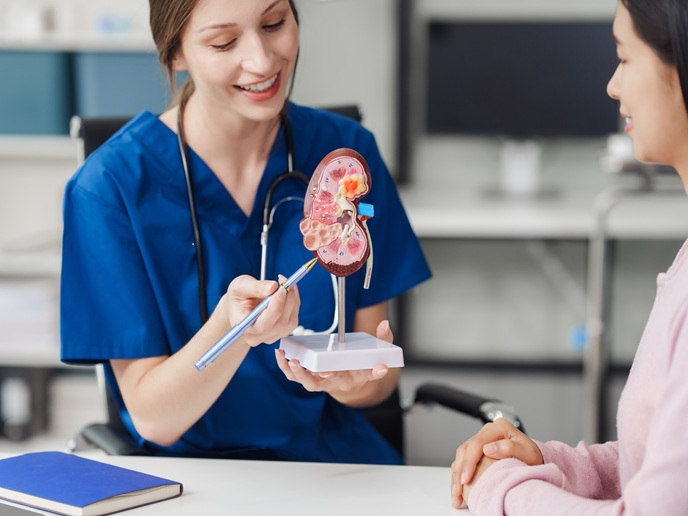
Screening for vision and hearing disorders in children is a highly effective means of avoiding long-term disabilities. Detecting and treating a lazy eye in early childhood, or a hearing impairment in newborns, can avoid a lifetime of visual impairment or delayed speech and language development. “Screening programmes differ greatly regarding age of screening, tests used, screening location and what professional conducts the examination,” notes EUSCREEN(opens in new window) project coordinator Huib Simonsz from Erasmus University Rotterdam(opens in new window), the Netherlands. “Vision and hearing screening is often only available in high-income countries.”
Screening situation uncovered
The EUSCREEN project first took a snapshot of current screening across Europe, to identify shortcomings and develop tools for improvement. An ambitious survey of 46 countries was conducted to gather data on prevalence of a lazy eye and hearing impairment, screening age, screening tests, coverage and attendance. It also looked at screening professionals, referral rates, lack of follow-up, treatment, screening costs and more. “For vision, we found that 13 different types of professionals screen,” says Simonsz. “For measurement of visual acuity between age 3 and 7, 35 different charts with pictures or numbers are used.” When it comes to hearing, the survey found that universal newborn screening is carried out in 26 high-income countries and in three low- and middle-income countries. It also revealed that the frequency of screening and the choice of screening method are strongly related to health expenditure and the human development index. An online cost-effectiveness model(opens in new window) for the introduction or modification of a screening programme was developed. Healthcare providers and policymakers can enter a variety of parameters – screening test, age, frequency, location, professional, etc. – in order to calculate the cost and effectiveness of a screening programme.
New programmes introduced
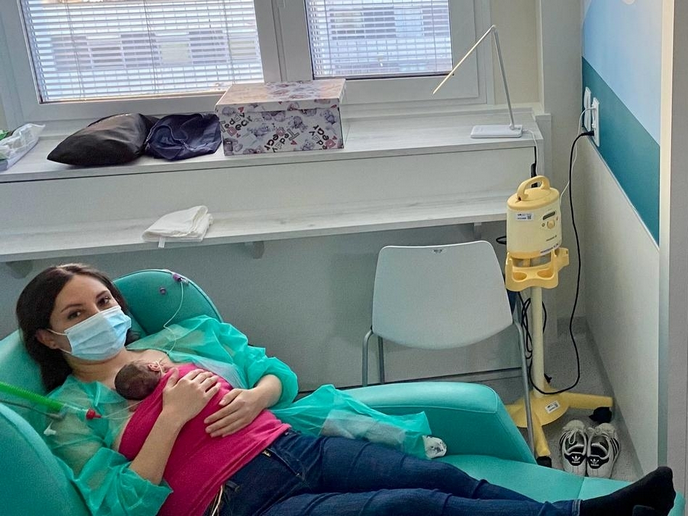
The ultimate goal of the EUSCREEN study was to compare the cost-effectiveness of screening programmes across borders in Europe. The cost-effectiveness model can do that, but it relies on accurate and available input data. The survey, however, unveiled a great lack of monitoring, data collection, quality control and evaluation, even in the most developed screening programmes. “The 10 variables essential for calculation of cost-effectiveness of screening programmes are not known or recorded in most countries in Europe. Recording these is essential, as the inability to compare screening programmes causes the diversity and inefficiency to remain,” adds Simonsz. The project also introduced vision screening in Romania and hearing screening in Albania. “We thereby identified requisites, facilitators and barriers regarding screening,” explains Simonsz. In Cluj County in Romania, visual acuity was measured in children at age 4 or 5. “In the cities, screening by resident nurses in kindergartens went very well,” remarks Simonsz. “In rural areas, however, kindergartens are small and screening was difficult.” A travelling screening nurse was employed, and successfully screened many children in rural villages. In Albania, newborns were first screened after birth in the maternity clinic, a process that worked very well. For subsequent screening examinations, the parents had to return to the clinic. However, due to travel distances, some follow-up did not take place. This underlines the need to keep track of infants with good administration, supervision and monitoring. A Manual(opens in new window) for implementing or modifying screening programmes sums up the entire expertise gained in the study. “This serves as a guide,” says Simonsz. “It contains chapters on planning screening, governance, local contexts, practical implementation of screening, public communication and monitoring.”