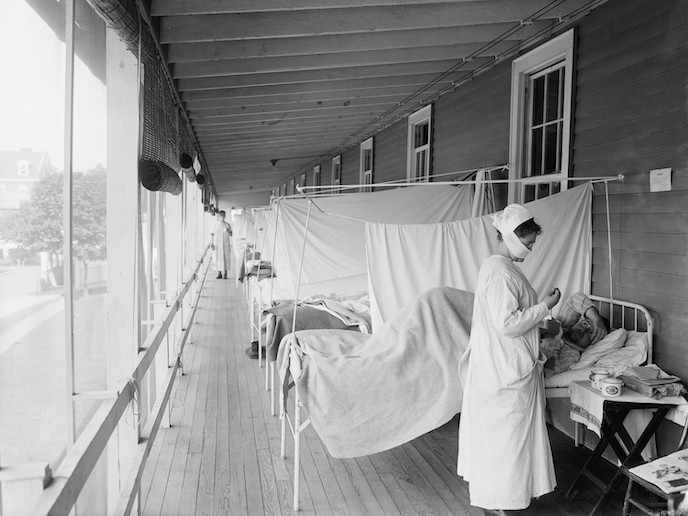
1918 Spanish flu pandemic provides clues on social factors behind spread
The DIS2 project looked at disability as a risk factor during the 1918 Spanish influenza pandemic, which affected one third of the global population and killed millions, to try to understand both biological and social reasons for differences in the number of cases and deaths. “We can then use that to hopefully inform pandemic preparedness today,” says researcher Jessica Dimka, co-leader of the Centre for Research on Pandemics and Society(opens in new window) at Oslo Metropolitan University, Norway. “Of course, I was not expecting the [COVID-19] pandemic,” she adds, having started the 2-year research project(opens in new window) in June 2019 with the support of the Marie Skłodowska-Curie Actions(opens in new window) programme. This made the work even more topical. The current COVID-19 pandemic has also highlighted the importance of underlying conditions in the disease outcomes, she notes.
How Spanish flu spread
Dimka delved into the National Archives of Norway, including census records and reports from psychiatric hospitals and residential schools for disabled children. She then looked into the Demographic Data Base at the Centre for Demographic and Ageing Research(opens in new window) (CEDAR) at Umeå University, Sweden, which includes 1918 parish records on the general population, to compare with wider exposure to Spanish flu. “In almost all the reports it was felt the disease was introduced by a staff member in institutions. This makes sense as they’re the ones who are going to be in the community,” notes Dimka. “There were reports that slightly more than half the staff reported cases while around 25 % of patients were affected.” However, patients in institutions had a higher chance of dying of the disease, with a 10 % fatality rate compared to 1 % among staff. “It does show some kind of susceptibility of the patients. They were less likely to be exposed to the disease or develop it but once they got it, they were more likely to die,” remarks Dimka, a biological anthropologist. Those with psychiatric and intellectual disabilities had a higher chance of dying, she found from the database records. However, there was no difference with other types of disabilities, including physical disabilities, compared to non-disabled people.
Simulation model
Behaviour and demographics data based on the historical research was used to build an innovative computer simulation model of a school for children with disabilities similar to the ones in the Norwegian archives. “It had different spaces, like classrooms, dormitory rooms and external spaces. And I had information on their daily schedules,” Dimka explains. “The disease was introduced [in the model] to see how it spreads, modelling different behaviours such as changing who was the first case and changes in the different disease parameters.” “The model showed that, if the first case was a staff member, cases among staff spread earlier. But if students got it first, disease spread rapidly and then the staff were affected a little bit later. That gives us some insights into what you might do to try and stop the spread of an epidemic by limiting introductions,” she adds. This project was the first to focus on disability as a risk factor for morbidity and mortality during historical pandemics, she says. “This helps with current or future pandemics – you can’t just think about medical risk factors, but also how they interact with social factors.”