Improved breast cancer diagnosis on the tip of a needle
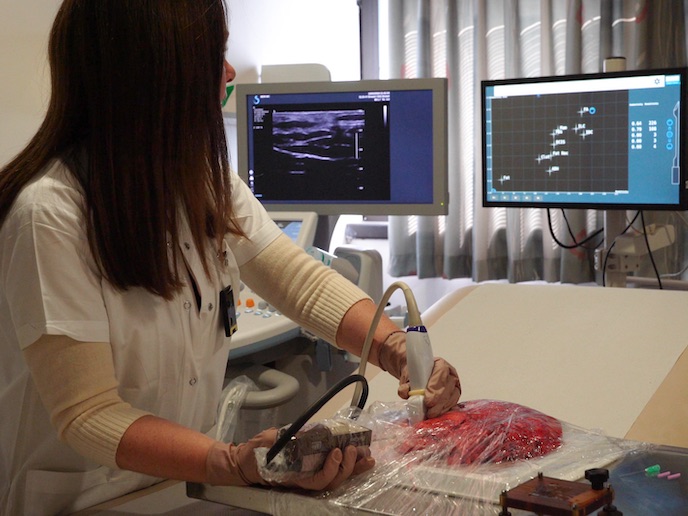
The SmartGuide project has developed a device based on radio frequency (RF) technology that instantly analyses human tissue using electrical sensors on a biopsy needle. The first-of-its-kind device guides the physician to the most suspect area for an accurate evaluation of disease. “A percentage of women undergoing mammography breast cancer screening will have a suspicious result and will need a tissue biopsy in order to get an accurate diagnosis by pathologists,” explains Mr Gal Aharonowitz, chief operating officer and general manager of Dune Technologies(opens in new window) in Israel, the firm which developed the device. The device uses RF technology to analyse the biopsy tissue. “Different types of tissue differentiate themselves by their electrical properties which our technology can measure in real time,” he says. The readings are displayed on a ‘tissue map’ and classified using a proprietary algorithm developed by the company from previous data sets of electrical properties that were correlated to types of tissues. The map of the tissue types that are in contact with the sensors embedded along the biopsy needle is presented to the radiologists during the procedure. More accurate biopsies “SmartGuide does not replace pathological analysis, but rather guides the radiologists to the most suspicious tissue to enable more accurate biopsy and pathology,” Aharonowitz says, adding it reduces the number of false negatives and false positives, avoiding misdiagnoses of patients and the need for repeat biopsies which currently affects 18 % of breast cancer patients. “This improved accuracy of pathology also significantly reduces healthcare costs,” he says. The RF tissue characterisation technology is currently used in the company’s MarginProbe device, which enables surgeons to identify microscopic residual cancer on the external layer of freshly excised cancer during lumpectomy procedures, and if required, to remove additional tissue during surgery. It reduces the need for repeat surgeries by 56–79 % and is in routine commercial use in over 70 hospitals in the United States and Israel. The EU project extends its use to an earlier stage of breast cancer treatment – early detection. “We took an off-the-shelf biopsy needle and embedded the RF sensing technology on it,” says Aharonowitz. “Once you insert the needle into the tissue you immediately and continuously have a response from each of the sensors.” The technological challenge Miniaturising the sensors to one-tenth their previous size to enable them to be embedded on the needle and receive accurate measurements without interference from the surroundings was a huge challenge. “Initially we only had feasibility studies from testing the sensors on an outer surface of the tissue. We didn’t have an understanding of whether we could measure the tissue with sensors on the biopsy needle when the needle is inserted into the tissue. No one in the world had successfully done that before,” Aharonowitz says. “We developed proprietary hardware and software which needs to perform accurately and instantaneously because of its real-time requirement.” Ex-vivo trials using extracted tissues demonstrated the device can detect tissue types, including malignant tissue, and differentiate between healthy and cancerous tissue with 84 % accuracy, a highly success rate for this stage. In vivo human clinical trials have begun involving patients undergoing breast biopsy procedures.