Functional precision oncology for colorectal cancer
The notion of personalised medicine will celebrate its 20th birthday in 2023, the result of the finalisation of the Human Genome Project(opens in new window). Along with this scientific triumph came the promise of personalised medicine. Today, only about 30 % of cancer diseases have a genetic component that indicates a certain treatment, so roughly two thirds are still without actionable markers. To make up for this shortfall and to ensure cancer patients receive effective treatments, the EU-funded MicroCaT(opens in new window) project tested a novel functional precision approach to guide colorectal cancer treatment.
“We do for cancer what antibiograms do for infection”
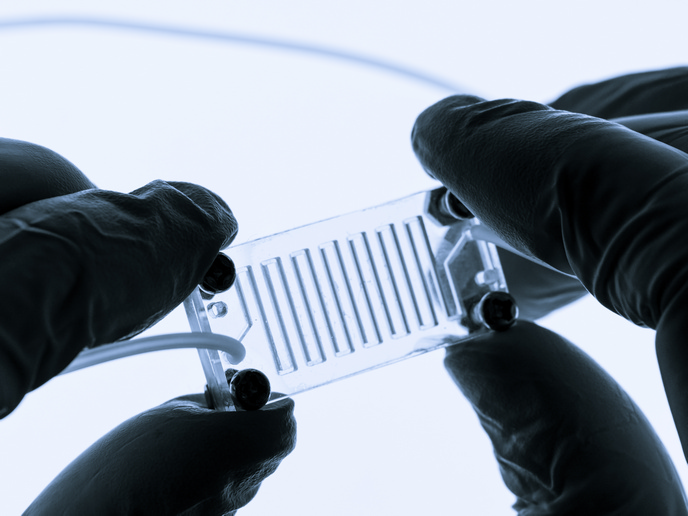
“In a nutshell, our strategy complements the genomic characterisation of tumours with functional data on their resistance and sensitivity to drugs,” outlines Ole Thastrup, founder and CSO of host company 2cureX, a Danish SME. The revolutionary new test is called IndiTreat® and involves thousands of 3D miniature tumours grown from the patient’s cancer tissue. See micro tumour in the image above. Each micro tumour is subjected to combinations of available drugs so the best possible treatment option can be selected. The cancer cells under scrutiny display in vitro the same behaviour as the patient’s tumour. “This is so groundbreaking. We have gone from a ‘hit and miss’ approach based on tumour characteristics to functionally guided treatment with a very good chance of working,” states Thastrup. The advantages of using IndiTreat® are overwhelming. Administration of several rounds of drugs is expensive for hospitals and health departments. For patients, there is an increased number of unwanted side effects for every round of new drugs and a risk that the disease will progress further. Knowing in advance if the tumour is resistant to the treatment would enable a completely new way of approaching treatment decisions.
Rigorous yet successful clinical trials
The main MicroCaT objective was to clinically validate IndiTreat® and expand its commercialisation. For the clinical study, 45 patients with Stage IV colorectal cancer were recruited and monitored at Vejle University Hospital, one of the major Danish cancer centres. “The bar was set extremely high,” Thastrup recalls. “The hospitals were prepared to run the study and carry a significant part of the cost. This was nerve racking as the hospital investigator was in charge and defined the clinical endpoint, in this case, it was set to increase the number of patients that did not experience progression of their disease after eight weeks of treatment by 100%. “The good news is that we were able to beat the endpoint by improving patient outcome by 150%.” This was a highly successful outcome for the first interventional clinical trial where the treatment is guided by 3D micro-tumours. The subsequent marketing based on these clinical results is on a very firm footing. “We are very thankful to the resident oncologists for not only defining and running the clinical trial; but also assisting in solving problems in this all new clinical setting,” adds Thastrup. In parallel with the clinical trial, 2cureX received an ISO certification and CE marked IndiTreat®, meaning 3D micro-tumours can be brought into routine clinical practice. As Thastrup comments: “This is an important milestone for us and shows the high degree of product design, development and manufacturing activities.”
Significant impact on cancer treatment
2cureX has started additional clinical studies with leading cancer hospitals in ovarian and pancreatic cancer. “These cancers are among the ‘big ones’ in terms of mortality,” Thastrup notes. Colorectal cancer is the second biggest cancer killer in Europe, with an estimated 175 000 deaths in a year, and pancreatic cancer is the third leading cause of death from cancer. The work on IndiTreat® continues with the Horizon 2020 project DECIDER(opens in new window). “Focusing on mechanisms behind drug resistance in ovarian cancer, the project is also looking into regulations on personalised medicine and how patients can benefit from research results as quickly as possible,” Thastrup concludes.