Precision immunotherapy, a game-changing treatment for sepsis
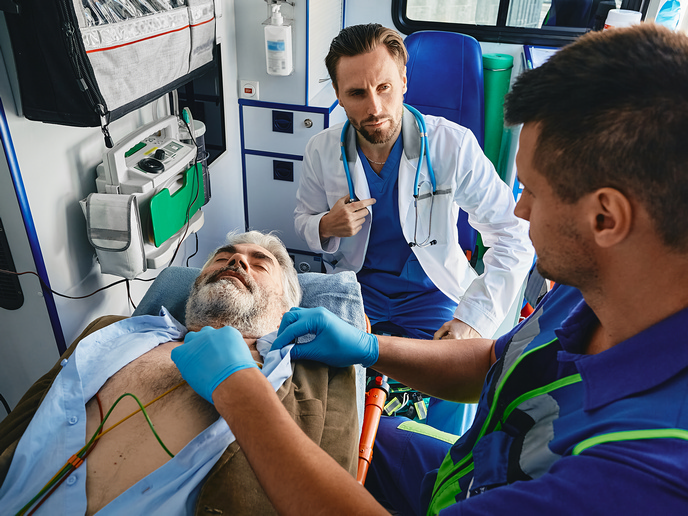
Sepsis is a life-threatening condition where the patient’s immune system has a dysregulated response to infection. Individual components can react too aggressively (macrophage activation-like syndrome (MALS)) and too weakly (sepsis-induced immunosuppression (SII)) at the same time. Recent figures show a dramatic rise in prevalence, with an estimated 166 million cases globally, and around 21.4 million sepsis-related deaths annually(opens in new window). Current sepsis treatments – such as administrating fluids, broad-spectrum antimicrobials, low-dose corticosteroids and insulin for glycaemic control – do not target the underlying cause. While immunotherapy to enhance the patient’s own innate immune response has to date constituted a possible alternative therapy to the current treatment, many clinical trials have failed to demonstrate their effectiveness for sepsis patients. “This is likely due to the sheer diversity of immune system dysregulation, with the condition manifesting differently across patients, highlighting the need for a more precise approach,” says Mihai G. Netea, coordinator of the ImmunoSep(opens in new window) project. The work aims to develop personalised immunotherapy treatment at Radboud University Medical Center(opens in new window), the project host. “Our findings reinforce the promise of precision immunotherapy, if informed by immuno-profiling,” Netea adds.
Reversal of immune dysfunction
The ImmunoSep project conducted a double-blind, placebo-controlled, randomised, phase 2b (proof of concept) clinical trial across six countries: Germany, Greece, Italy, the Netherlands, Romania and Switzerland. The 276 selected adults were affected by either pneumonia sepsis or primary bacteraemia sepsis. Over 15 days, half the participants received precision immunotherapy – the anti-inflammatory drug anakinra for MALS, or immune stimulant interferon-gamma for SII. The remaining half received a placebo. Targeting MALS and SII was found to improve organ dysfunction by day nine, compared with placebo. Differences were also found in overall improvement in organ dysfunction by day 15, accompanied by reversal of immune dysfunction and resolution of the underlying infection. The team recorded a 6.1 % absolute decrease in 28-day mortality. “These positive results open up exciting new avenues for treating sepsis patients with personalised medicine ,” notes Netea. “And given that the drugs were first administered 36 to 48 hours after the onset of sepsis, reducing this delay may boost future results even further.” The full results(opens in new window) of the ImmunoSep trial were published at the end of last year in the ‘Journal of the American Medical Association’, one of the most prestigious scientific journals in the world. Patient samples were also collected for genomic, epigenomic, transcriptomic, metabolomic and proteomic analysis to identify immune biomarkers useful for future diagnosis and treatment. “This data could help identify subgroups of sepsis patients with dysregulation in specific components of the immune response, called ‘immune endotypes’,” explains Netea. “For each, we will identify the body’s disease mechanisms and potential therapeutic targets.”
Machine learning and multi-omics
The high prevalence and mortality rates of sepsis, with MALS and SII profiles present in many patients, are reflected in ongoing efforts to find innovative diagnostic and treatment options. “The COVID-19 pandemic prompted a surge of interest in precision immunotherapy for severe infections, with anakinra registered to treat COVID-19 patients with pneumonia,” says Netea. Inspired by reports from others that machine learning and multi-omic approaches could improve the detection of immune dysregulation profiles, the team is now identifying biomarkers to build an algorithm able to classify sepsis-related immune responses, for use in hospitals. “We want an alternative to the current methods of identifying subgroups of sepsis patients that are reliant on advanced lab equipment and specialised personnel,” explains Netea. “In our trials, the majority of screened patients were excluded as their immune state was unclassified, suggesting that the biomarkers used – ferritin and HLA-DR – do not adequately capture the range of immune dysregulation. We need something more sophisticated but still user-friendly.”